Campaigners have slammed Britain’s top GP after he defiantly dismissed calls to give all patients the right to face-to-face care.
Professor Martin Marshall, chair of the Royal College of GPs, yesterday told MPs that patients who ‘absolutely need’ to be in the same room as their doctor are still being seen.
But Covid safety measures and sky-high demand mean it is not possible to offer in-person consultations to people simply because they would ‘like’ one.
Professor Marshall said it was an impossible ambition to deliver and insisted the rate of online consultations, via telephone or online, is ‘about right’. Just over half of all GP appointments are now carried out in-person, NHS figures show.
Grilled by MPs on the Health and Social Care Committee about the lack of face-to-face appointments, he also admitted that the traditional concept of a full-time GP was dying.
He said it was ‘something we won’t see again’, saying that three-day weeks for family doctors are here to stay. Professor Marshall also claimed that part-time GPs were still working 12 hours days under ‘intense pressure’ and that adding any more to their pile could be dangerous for patients.
Professor Marshall said: ‘General practice across the board introduced remoted working in two to three weeks in March of last year, so it’s hardly surprising that it’s taken time for clinicians and patients to get used to it.
‘But I do suspect patients will get used to it. I don’t think we’ll go back to 80 per cent of consultations at general practices being face to face.’
But last night, Dennis Reed, from Silver Voices — a campaign group for the over-60s which is demanding a legal right for patients to have a face-to-face appointments — hit back at Professor Marshall.
He accused the GP of ‘shrugging his shoulders and surrendering before the battle is over’.
Mr Reed added: ‘He needs to keep on fighting for more resources so we can all get the care we need.’


Martin Marshall (left), chairman of the Royal College of GPs, told MPs that patients who ‘absolutely need’ to be in the same room as their doctor are being seen. Right: Francine Jury spent 28 minutes repeatedly calling her surgery before reaching the receptionist
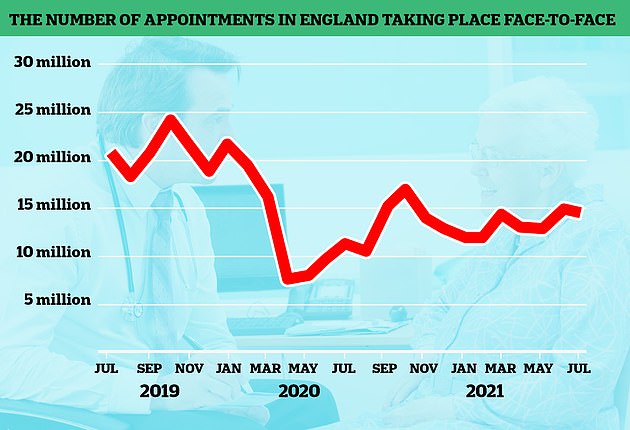
In-person appointments began to increase last summer, before dropping again during the second wave. Despite being on the rise, the figures are still much lower than pre-pandemic levels

Up to March 2020, around 80 per cent of all appointments across England were in-person, but this dropped to 46.8 per cent last April and has not risen above 57 per cent since
Doctors urged to cut prescriptions
Doctors have been urged to slash the number of prescriptions given to patients.
A staggering 15 per cent of adults take five or more medications a day, a major government review has revealed today.
And 10 per cent of the drugs prescribed by GPs are inappropriate or not needed.
The crisis means thousands of elderly patients are ending up in hospital due to the harmful side-effects of drugs they did not need to take in the first place.
Today’s report into overprescribing, led by the chief pharmaceutical officer for England Dr Keith Ridge, contains recommendations on how to tackle the issue. Doctors have been told to step up ‘social prescribing’ – when patients are referred to community, non-clinical services – and to send them for gardening or art classes as an alternative to medicines such as anti-depressants.
NHS staff will also be urged to work with pharmacists to launch regular reviews of medications and to ensure that patients are not taking pills just for the sake of it.
The review also said GPs must cut down on issuing prescriptions to tackle climate change. It said 25 per cent of the NHS’s carbon footprint is due to medicines, mostly due to manufacturing and the supply chain.
The report found that about one in five hospital admissions in over-65s are caused by the adverse effects of medicines.
The more pills a person takes, the higher the chance of an unwanted or harmful effect.
For example, some medicines, such as those to help reduce blood pressure, can also increase the risk of falls among the frail and elderly.
Some 7 per cent of a dults take eight or more prescription drugs a day, the review found. It said 1.1billion prescription items were dispensed in England last year and as many as 110million may have been overprescribed.
The report follows concerns that millions have become hooked on prescription pills, such as anti-depressants and painkillers. The Daily Mail has long-campaigned for greater recognition of the prescription drugs addiction crisis.
The review also said the NHS must provide clear information on how to withdraw from prescription pills. The Government said it has accepted all recommendations and will now begin work to implement them. Health Secretary Sajid Javid said: ‘With 15 per cent of people taking five or more medicines a day, more needs to be done to listen to patients and help clinical teams tackle overprescribing.’
And Dr Ridge said the ‘report will help clinicians ensure people are getting the right type and amount of medication, which is better for patients and also benefits taxpayers’.
Advertisement
Mr Reed told The Daily Telegraph: ‘It seems to me really arrogant to suggest the level of face-to-face appointments is about right when we are hearing so many accounts of patients — especially elderly ones — suffering and unable to get the help that they need from their GP.
‘We need to get back to at least the levels of before the pandemic.
‘We are hearing too many accounts of patients pleading and pleading to see their GP, doing battle with receptionists, and only able to get an appointment by phone or online.
‘The practice of “remote first” appointments is inherently unsafe and bound to miss symptoms.’
It comes as the UK’s biggest medical union demanded a meeting with Sajid Javid to discuss the criticism doctors are facing because of the drop-off in in-person care.
The British Medical Association (BMA) said doctors have received a ‘wave of abuse’ from patients over the lack of face-to-face appointments.
It has called for an urgent meeting with Health Secretary Sajid Javid to resolve the issue.
The union insisted that claims that GPs were refusing face-to-face appointments were ‘inaccurate’ and ‘dangerous’.
In a letter to the Health Secretary, the BMA said family doctors were still seeing patients in person ‘when this is needed’ and were using telephone and online consultations otherwise.
But anxious patients have struggled to even reach a receptionist when calling their doctor, with one woman claiming she rang 673 times before she was able to get through to someone.
Francine Jury, from Manchester, spent 28 minutes repeatedly calling her surgery before reaching the receptionist.
Professor Marshall acknowledged the proportion of patients seen in surgeries has fallen from eight in ten before the pandemic to less than six in ten now.
He added: ‘I don’t think we’re going to go back to 80 per cent being face to face.’
His appearance in front of the Commons health committee yesterday came just a day after the Daily Mail launched a campaign to improve access to family doctors.
The Mail is demanding face-to-face GP appointments are the default, and that anyone who wants to see their family doctor in-person should be able to do so.
Incentives should be provided for local surgeries if necessary.
This newspaper is also calling for the Government to deliver on its election promise to recruit 6,000 more GPs and provide 50million more appointments a year.
Experts have been demanding action amid fears that cancers and other serious health conditions are being missed remotely.
Boris Johnson and Health Secretary Sajid Javid are among those pushing for the return of more in-person care.
Caroline Abrahams, of charity Age UK, backed calls for increased investment in GP services and warned that pensioners had been left feeling ‘cast adrift’.
She said: ‘This is not acceptable and we have to change it fast, to regain public confidence and reassure them that whoever they are, they will not be left behind.’
Senior Tories also backed the campaign. Former Tory leader Iain Duncan Smith said: ‘It’s really important for GPs to try to get back to face-to-face appointments because that is so vital for the health of older people in particular.
‘The default should be face to face.
‘GPs are not seen like the rest of the health service – we talk about them as family doctors. They are people that can be trusted, who see you as a human being.

Professor Marshall said about 80 per cent of GP appointments were conducted face to face prior to the pandemic, dropping to 10 per cent in the first wave. Now this figure is around 56 per cent
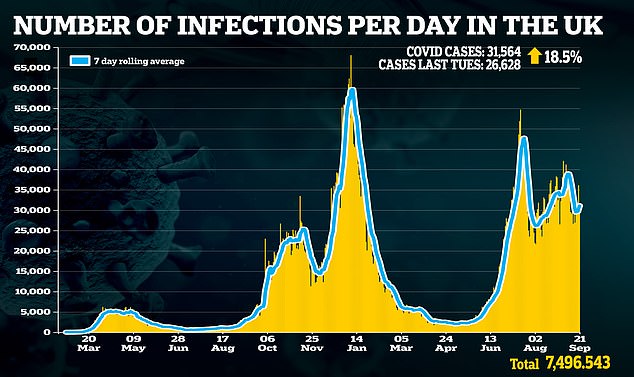
Professor Marshall added that remote consultations continue to play a role in reducing the spread of coronavirus

Professor Marshall acknowledged the proportion of patients seen in surgeries has fallen from eight in ten before the pandemic to less than six in ten now. But he insisted the rate of online consultations, via telephone or online, is ‘about right’
Culture of part-time work fuels staff crisis
By Shaun Wooller Health Correspondent
The general practice crisis is being fuelled by more family doctors working part time and retiring early, Britain’s top GP said yesterday.
Martin Marshall said the profession was attracting recruits and all training places were full but ‘the plug is out of the bath’.
He said young medics now wanted a ‘portfolio’ career where they worked part time and did jobs alongside general practice. But this means full-time GPs are ‘probably something that we won’t see again’, the chairman of the Royal College of GPs added. His comments to the Commons health committee came after figures revealed the average GP salary has soared to £100,700 – three times that of a nurse. Family doctors taking early retirement are now drawing their pension at an average age of 57, NHS officials say.
Figures show fewer than one in four fully qualified GPs work full time. Professor Marshall added the trends are due to general practice being ‘a highly pressurised job’.
Advertisement
‘The Government has to get more GPs as they are the most important part of the NHS. But that peculiar link between GPs and patients relies on trust – and that is more difficult when the meeting is not face to face.’
Andrew Selous, Tory MP for South West Bedfordshire, said one of his constituents called his surgery 99 times before he got an appointment. He urged the Government to boost recruitment, as well as retaining older GPs.
Mr Selous said: ‘We’re getting more GPs in at the bottom but we are losing experienced partners at the top. I have raised the need for the Government to recruit more doctors to be GPs as well as what we need to do to retain more GPs.’
Professor Marshall told MPs that there are patients who ‘absolutely need to have face-to-face contact in order to get the high quality care to pick up the right diagnosis’, while others simply ‘like’ in-person appointments and GPs do not have the capacity to deliver this.
He said: ‘People are saying the patient should have a right. There’s no point in having a right if it’s undeliverable and it is essentially undeliverable at the moment.’
He said GP workload had gone up during the pandemic ‘and indeed over the last decade’, adding: ‘The pandemic isn’t over. We’d like to think it is. It might be over for pubs and nightclubs [but] it’s not over for health services.’
Professor Marshall said about 80 per cent of GP appointments were conducted face to face prior to the pandemic, dropping to 10 per cent in the first wave. Now this figure is around 56 per cent.
He told MPs 56 per cent is ‘where we should be’, adding that face-to-face appointments ‘aren’t needed by everybody’.
Professor Marshall said there is a ‘risk’ that serious illnesses are being missed as a result of GPs conducting more remote consultations. But he thinks it is happening ‘less’ now than at the start of the pandemic as doctors have learned who they need to see in person.
He added: ‘When you need to examine somebody or do a blood test, it’s obvious you need face-to-face appointments. The greater challenge is for the softer reasons for face-to-face consultation. So when I see a patient in my room who I don’t need to examine but I can see, for example, is anxious, or I can smell alcohol on their breath, or they’re dishevelled and they’re usually well-kempt, those are all soft signs that help me make a better diagnosis.
‘So face-to-face appointments are important when they’re needed. My point is they’re not needed for everybody.’
Professor Marshall added that remote consultations continue to play a role in reducing the spread of coronavirus.
Heartbreaking stories lay bare the perils of remote diagnosisMy cancer fears were right… but it was too late
By Liz Hull

Suspicions confirmed: Steve McGregor with Pam and Alex
A former paramedic who feared he had cancer was refused a face-to-face GP appointment – only to be told it was terminal eight months later.
Steve McGregor, 48, a biologist who retrained to work for the ambulance service after 20 years in cancer research, first suspected that his breathing difficulties were something sinister.
But despite 20 calls starting in March last year, his GP at Trinity Medical Centre, Stoke-on-Trent, refused to see him during lockdown and dismissed his symptoms as anxiety and asthma.
In desperation, in May 2020 Mr McGregor walked into A&E at his local hospital, where he was also told there was nothing wrong.
Only when the father of one threatened to sue his GP was he referred for a scan in October, which revealed he had stage four lung cancer that could not be cured. Last night Mr McGregor said: ‘I have a knowledge of healthcare and science but still I couldn’t get a referral, so what hope is there for Joe Bloggs?’
In January this year, Mr McGregor married his partner, Pam, 48, with whom he has a son, Alex. Mr McGregor said: ‘I fully support the Daily Mail’s campaign, people must get appointments face to face if they want them.’
Mr McGregor’s GP Dr Bhalchandra Narayan Kulkarni previously said: ‘For reasons of patient confidentiality the practice is unable to discuss any aspects of patient care.’
Soul mate was fobbed off by GPs and suffered months of delays
By Gregory Kirby

Mr Stokes, 74, said his wife of 46 years was ‘constantly fobbed off’ by reception staff at the Wiltshire surgery when she tried to see a doctor in the pandemic

Nick Stokes, who sadly lost his wife, Joy, to cancer, at his home in Worton, Devizes, Wiltshire.Also pictured is his dog, Bailey
An ‘OUTRAGED’ former NHS trust chairman whose ‘soulmate’ died of cancer after struggling to secure in-person appointments has urged patients not to be ‘fobbed off by GPs’.
Nick Stokes’ wife Joy, a 69-year-old former PE teacher, died of breast cancer this April after an ‘avoidable’ six-month diagnosis delay. In phone consultations, her GP said she had arthritis associated with ‘getting older’.
Mr Stokes, 74, said his wife of 46 years was ‘constantly fobbed off’ by reception staff at the Wiltshire surgery when she tried to see a doctor in the pandemic. Mrs Stokes, who loved hockey, athletics and golf, had survived breast cancer in 2006.
The grandmother tried to see a GP in May last year after developing persistent leg and joint pain. She saw an NHS physio and a private one in her hometown of Devizes, Wiltshire, in October.
It took until mid-January this year for Mrs Stokes to see her GP in person and after tests she was diagnosed with advanced breast cancer which had spread to her bones and brain. She died on April 11, too ill to start chemotherapy. Her oncologist at the Royal United Hospitals, Bath, told Mr Stokes she may have survived if the diagnosis was earlier.
The former chairman at a Midlands NHS Trust, who could not visit her in hospital due to Covid, said: ‘I hate to think what went through her mind in those last weeks.’ Mr Stokes is now backing the Mail’s campaign as a ‘legacy’ to his wife.
400 phone calls to get through to the surgery
By Alex Ward
Patients are calling their GP surgeries up to 400 times to get through – only to be told they cannot have a face-to-face appointment with their doctor, it has emerged.
One individual who needed to change some of her husband’s cancer medication said she rang 390 times before her call was answered.
And Mark Cahillane, 63, from Swindon, Wiltshire, claimed he and his wife rang their local practice Ashington House Surgery 269 times before they got through.

In another shocking case, a woman called Abbey Meads Medical Practice in Swindon nearly 400 times trying to get her cancer-suffering husband a face-to-face appointment
His wife had been experiencing problems with her ankle. Mr Cahillane said he had been given ‘the run around’ in his efforts to get an appointment.
He said: ‘My wife rang on the landline and it took 45 minutes before she could get through. And then the receptionist was saying that they can’t make a face-to-face appointment until we speak to a doctor. You’re just going around in circles.’
They called the surgery the following day and waited another 55 minutes before they finally managed to speak to a member of staff. Mr Cahillane added: ‘Then there’s a call queue which was another 15 minutes.
‘And again, they said they can’t do a face-to-face appointment, ‘you have to wait for a doctor to call you’…
‘You’re trying to get things sorted out because the NHS is trying to catch up on the backlog of patients. My wife has a very bad ankle and it’s serious and she needs to get it sorted out.
‘I was trying to be polite and calm. It was as stressful as anything.’ Mr Cahillane said while his wife was forced to wait for hours to be contacted, they were pleased with their conversation with the doctor.
In another shocking case, a woman called Abbey Meads Medical Practice in Swindon nearly 400 times trying to get her cancer-suffering husband a face-to-face appointment. The woman said her husband had needed an appointment with his family doctor in order to change his medication.
She said: ‘I just redialled for 390 times – but before I’ve had over 425 – and then you get put in a queue and you still have to wait.’ It took her three days to finally get through to an operator and book an appointment.
Great Western Hospitals NHS Trust, which is responsible for the running of the Abbey Meads surgery, apologised and said the delays had been the result of ‘significant pressure’ on their staff.
Dean Mills, assistant practice manager at Ashington House Surgery, said the pandemic had seen new working methods introduced.
He said: ‘Patients can play their part in easing the pressure by calling outside of the busiest times, such as first thing in the morning, and making use of alternative healthcare services, such as NHS 111 and local pharmacies.’
Twice in my life, I’ve been saved by my GP. Would I still be here if I hadn’t seen them face-to-face, asks SARAH VINE
Twice in my life I’ve owed everything to a GP — once when my son was a baby and a few years later when I had peritonitis.
The doctors’ experience and quick-thinking made the difference between life and death. Both have since retired, but I owe them an inestimable debt of gratitude.
It is because of those experiences, and other smaller, equally memorable ones, that I am a huge supporter of general practice. GPs are vital, the linchpin of the nation’s health. Their contribution is invaluable.
But here’s the thing. Had I not been able to take my son to see the GP face to face, it is possible his illness — mastoiditis — would not have been detected. Thanks to antibiotics it has become, as the doctor said then, a disease you only really read about in medical textbooks.

Twice in my life I’ve owed everything to a GP. But had I not been able to take my son to see the doctor face to face, it is possible his illness would not have been detected (stock image)
It was certainly the first case he had seen, despite being a seasoned practitioner. Even with a physical examination the problem is hard to spot. Luckily he did, and my son — then just a few months’ old — was rushed to our local hospital, and then St Thomas’ in London, where surgeons drilled a hole in his head to drain an abscess on his brain caused by the infection.
And it was a similar story with my leaky appendix. I’d had stomach pains and vague sickness on and off. That day I woke feeling particularly icky, so rang the surgery and was given an afternoon appointment — which I almost cancelled when, at lunchtime, I felt perkier.
But I went anyway, said I was feeling a little better and my GP said she would have a general prod to be safe. She did her thing, then requested an ambulance. I spent the next two weeks in hospital recovering from a four-hour operation. I’ve never felt so ill in my life.
The outcome in both cases would have been very different had the consultations taken place by phone — or online. It was the human interaction that made all the difference.

The outcome in both cases would have been very different had the consultations taken place by phone — or online. It was the human interaction that made all the difference. Pictured: Sarah Vine
That is why the current situation, in which just 57 per cent of GP appointments are in person compared with 80 per cent before Covid, is not only unacceptable: it’s dangerous. And why this newspaper is so right to insist that we do better.
Dr Chaand Nagpaul, chair of the BMA council, can rant all he likes about Covid safety measures and ‘an onslaught of abuse and media scapegoating of GPs and their staff’. The fact remains: patients are suffering, even dying, and it is his job — and duty — to do something about it.
Of course, there are many brilliant practitioners out there, who, despite the obstacles, manage to offer first-class care. But it is a postcode lottery and shouldn’t be.
The fact Dr Nagpaul is so defensive is, in many ways, the root of the problem. There seems to be a fundamental refusal to accept the existence of a problem, let alone that he and his members should in any way be held accountable.
Instead of excuses, he should offer solutions. Instead of bleating about workload, he should find out why, if GPs are, as he claims, ‘seeing more patients than ever, working longer hours than ever’ it does not seem to be translating into adequate care.
Though he is referring to NHS appointments, many GPs are also seeing patients privately, as they are free to. Given the difficulties many patients have getting a slot with a GP and the number of private helplines springing up, I do wonder if there might not be some crossover.
Abuse is unacceptable, but many patients feel exasperated at being unable to see a doctor face to face.
Yet there are frustrations on both sides: my surgery, for example, has a long recorded message designed to put off as many callers as possible — and when you do finally get through, they’re about as helpful as a Soviet border guard. I’ve been trying to get an appointment for weeks. I’ve all but given up.
I still have huge respect for GPs, who do so much for us all and who have been a vital part of the fightback against Covid-19. But this relentless drive to move to a remote working model is not OK.
Of course there are times when a telephone conversation is appropriate — as when I had swine flu in 2008, my GP dealt with me remotely, prescribing treatment and antibiotics for secondary infection.
But as a general rule, people need to see their doctors. Normal service must be resumed as soon as possible. It is up to the BMA and No 10 to make it happen. Ideally before the forthcoming National Insurance rise reminds us of quite how much we’re paying for this shambles.
12,000 cancer patients suffer ‘unacceptable’ care hold-ups as NHS struggles to clear Covid backlogs, report finds
By ELEANOR HAYWARD HEALTH CORRESPONDENT FOR THE DAILY MAIL
Shocking delays in cancer care have left 12,000 patients facing ‘unacceptable’ waits to start treatment so far this year.
Analysis by Cancer Research UK has laid bare the extent of the worsening crisis facing patients as the NHS struggles to tackle the Covid backlog.
In the first six months of this year, just 72.8 per cent of cancer patients started treatment within the target of two months of an urgent cancer referral.
This means 11,568 patients have missed out on prompt diagnosis or treatment, damaging their survival chances.
The NHS in England says 85 per cent of patients should be seen, diagnosed and start treatment within two months of an urgent referral for cancer from their GP.
But the health service has missed this target for six years running and its performance is continuing to deteriorate.
The proportion of cancer patients starting treatment within two months has decreased for six years in a row.
In total over the past six years, 55,000 cancer patients should have been diagnosed quicker or started their treatment sooner.
In 2016, 82 per cent of patients were seen within this target – meaning around 4,000 missed out on quick care. But by last year this had fallen to just 75 per cent – with 14,600 facing delays.
Performance has been even worse this year as the Covid backlog continues to take its toll on services. Just 72.8 per cent of patients met the target in the six months up to July.
Early diagnosis and prompt treatment is crucial to survival chances. Every four-week delay in cancer treatment increases the risk of death by 10 per cent.
Cancer Research warned that pressure on the NHS is continuing to intensify as a result of a shortage of staff, and that without urgent funding survival rates are likely to fall.
One in ten diagnostic posts in the NHS are currently empty.
Michelle Mitchell, Cancer Research UK’s chief executive, said: ‘These figures are a stark reminder that cancer services have been struggling for years, with thousands of cancer patients having to wait longer than two months to get diagnosed and start treatment.
‘While NHS staff have been doing their utmost, the impact of Covid-19 and years of workforce shortages and insufficient infrastructure have meant that cancer targets continue to be missed. Cancer won’t wait and the time for the Government to fix these chronic issues is now.’
Professor Charles Swanton, Cancer Research UK’s chief clinician, added: ‘Being referred urgently because you might have cancer, receiving a diagnosis and beginning treatment are hugely anxious times for patients, which are further compounded when there are delays.
‘For people with cancer, every day counts; that is why we have cancer targets. I’ve been working in the NHS for a long time and it’s hard to watch the continuous deterioration, and the anxiety and worsening outcomes this can cause patients.’
Advertisement
Source link : https://www.dailymail.co.uk/news/article-10016079/Get-used-UKs-GP-says-face-face-appointments-WONT-pre-pandemic-levels.html