Boris Johnson last night piled pressure on GPs to offer more in-person consultations.
His spokesman said every patient had the right to a face-to-face appointment if they wanted one.
A day after the Mail launched a campaign to improve access to family doctors, Downing Street said: ‘The public rightly may choose to want to see their GP face to face – and GP practices should be making that facility available to their patients.’
Charities and politicians have been clamouring for the Prime Minister to act amid fears that cancers and other serious health conditions are being missed in remote consultations.
Just 57 per cent of GP appointments are now in person compared with 80 per cent before the pandemic.
‘The relationship between the GP and his or her patient really depends on face-to-face consultation,’ said Tory former health secretary Kenneth Clarke.
‘I find it difficult to see how anyone can diagnose totally accurately symptoms described over the telephone.
‘I think face-to-face appointments should go back to pre-pandemic levels and I don’t see why they can’t.’

A day after the Mail launched a campaign to improve access to family doctors, Downing Street said: ‘The public rightly may choose to want to see their GP face to face – and GP practices should be making that facility available to their patients.’
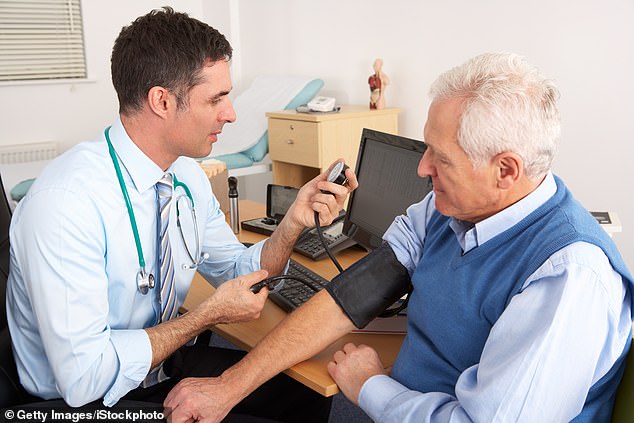
‘The relationship between the GP and his or her patient really depends on face-to-face consultation,’ said Tory former health secretary Kenneth Clarke. ‘I find it difficult to see how anyone can diagnose totally accurately symptoms described over the telephone
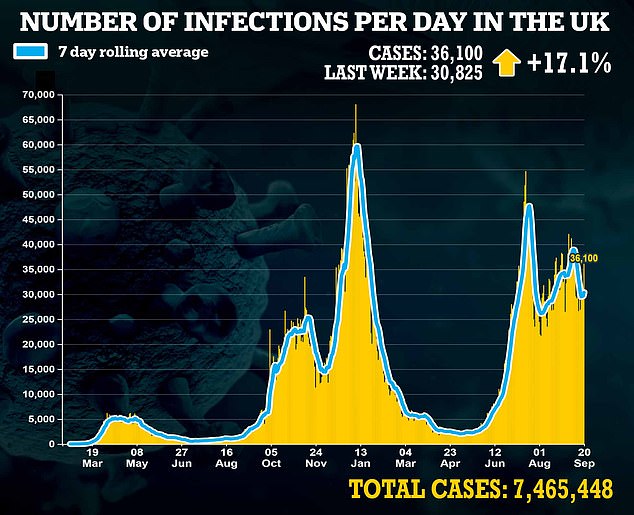
Just 57 per cent of GP appointments are now in person compared with 80 per cent before the pandemic
As the Mail’s campaign to restore in-person appointments to normal levels gathered momentum:
A study found patients given telephone appointments were more likely to end up in A&EIn one in five areas, face-to-face appointment rates are even lower than in JanuaryPrivate providers reported a rise in numbers paying for face-to-face accessMore stories emerged of patients developing serious conditions after struggling to see a GPThe BMA, the trade union for doctors, issued a robust statement insisting GPs were seeing millions of patients face to face every week
Doctors say telephone and video appointments allow them to get through more patients.
But critics believe the pendulum has swung too far and that doctors are more likely to miss the signs of a more serious illness if they don’t see someone in the flesh.

Pressed on the issue yesterday, the Prime Minister’s spokesman said: ‘The NHS has been clear to every GP practice that they must provide face-to-face appointments, and we fully support that

Caroline Abrahams of the charity Age UK said older people were struggling with telephone triage. She added: ‘We urge NHS England to challenge and support GP practices that have moved too far, too fast, in their use of technology.’
Pressed on the issue yesterday, the Prime Minister’s spokesman said: ‘The NHS has been clear to every GP practice that they must provide face-to-face appointments, and we fully support that.
‘GPs throughout the pandemic have worked hard to see patients and appointment numbers have returned to pre-pandemic levels.
‘It’s right that the public expect to be able to see their GP in person, if needed.’
Although the comments from Downing Street are a positive step, there has been no commitment to take action.
There have been calls to change the way GP practices are funded to incentivise doctors to see patients face to face.
The pressure group Silver Voices is campaigning for a statutory duty to be placed on them to hold in-person surgeries if patients want them.
Caroline Abrahams of the charity Age UK said older people were struggling with telephone triage.
She added: ‘We urge NHS England to challenge and support GP practices that have moved too far, too fast, in their use of technology.’
The BMA said: ‘The move to an initial telephone consultation to assess a patient’s needs was, and is, in line with NHS England’s and the Government’s guidance.
‘Many patients have really appreciated the benefit of alternative types of consultations, which can then be followed by a face-to-face appointment if needs be.’

Three case studies reveal to the Mail how they were affected by GPs reluctance to meet face to face
CASE STUDY ONE
I was fobbed off… then found I had a tumour
A new mum who suspected she had bowel cancer has told how she was ‘fobbed off’ by her doctor for months – before belatedly being diagnosed with the disease.
It then took a year before marketing worker Jenny Carter had surgery to remove a tumour.
The 37-year-old initially tried to get a face-to-face appointment in March last year when she was three months’ pregnant with her first child.
As her mother Christina was seriously ill with bowel cancer and she had an uncle suffering with the disease, she feared the worst when she experienced bleeding.
But her GP told her over the phone that she was too young to have bowel cancer and without seeing her, diagnosed piles – which is common in pregnant women.
The surgery had refused an appointment in person but in July 2020 agreed for her to pick up a stool-sampling kit.
When her sample was lost, Miss Carter, of Hornchurch, Essex, switched GPs – calling it ‘the last straw’.

Jenny Carter (pictured with daughter Penelope) was ‘fobbed off’ by doctors for months before being belatedly diagnosed and undergoing surgery to remove a tumour a year later. The 37-year-old initially tried to get a face-to-face appointment in March last year when she was three months’ pregnant with her first child.
Her daughter Penelope was born two months later and her mother died in November from the bowel cancer.
Although Miss Carter’s new doctor immediately took her concerns seriously, the pandemic backlog meant she could not have a colonoscopy until as late as February this year – almost a year after she first contacted her previous GP.
Medics found a malignant growth and the next month she had a tumour removed, which left her needing a life-altering stoma to process her waste.
She fears that if she had been she been examined in person a year earlier, she may have been spared the ordeal.
Miss Carter told the Mail how her first fears back in March 2020 were dismissed, despite recognising symptoms due to her mother’s illness.
She said: ‘I started experiencing the same symptoms I knew all too well like heavy bleeding and called my GP multiple times to express my concerns.
‘They said I was too young for bowel cancer despite knowing my family history. They said I had piles, which is quite common in pregnant women, without giving me an internal examination and gave me various creams to try but nothing worked.
‘It got to the point where I knew it was something more sinister. I called my GP in floods of tears but they told me they could not see me and if I had any problems I should go to the antenatal clinic. I was fobbed off the whole time.’
And she explained how devastated she was when the cancer diagnosis came almost a year later.
‘I knew it was going to be bad news when they asked me to come into a side room to discuss my results. My partner, Joel, was there with Penelope.
‘The doctor told me to sit down, but I didn’t want to. I just wanted to pace around the room. The doctor told me they’d found a “large suspected malignant lesion”. The rest was just a blur.
‘I was still grieving for my beautiful mum. I kept thinking I didn’t want to die. I had too much to live for.’
Miss Carter added: ‘It was only two days after my 37th birthday and my daughter was just five months old. I feel like I am on the road to recovery now. But when I had time to think about it after my operation I was very annoyed.
‘I have got a stoma now. If I had been diagnosed back in March 2020, I might not have needed such major surgery.’
CASE STUDY TWO
I cried down the phone, but still no appointment
Racked by a painful skin condition, a mother of three tried repeatedly to see her GP – only to be told: ‘If it’s that bad go to A&E.’
Jenni Payne, 42, said: ‘I suffer from psoriasis, which dramatically worsened last year in around August. I went from having one type of psoriasis to two and my condition was out of control.
‘I was calling the GP surgery, crying down the phone, but I was unable to get a face-to-face appointment.’

Jenni Payne, 42, said: ‘I was calling the GP surgery, crying down the phone, but I was unable to get a face-to-face appointment.’
Mrs Payne, who lives with her husband Richard and their children in Maidenhead, Berkshire, said: ‘Trying to get an appointment was impossible, even trying to get through on the phone was a nightmare.
‘It would take nearly an hour to get through to reception, who then tell you there are no appointments with the GP, not even phone appointments, and that I have to contact them via their online service.
‘I did this, filling in details about who I was, what my condition was, and why I wanted to talk to my GP.
‘The following day I got a call saying I needed to send images, so I got my husband to take photos and upload them. Fourteen weeks later and still not having heard anything, my condition had deteriorated so badly that nearly 70 per cent of my body was covered with psoriasis.
‘The skin on my back was so split that it was bleeding, but when I rang the doctor’s surgery I was told, “We have done all we can for you – if it’s that bad go to A&E”.
‘I thought to myself, this is ridiculous, I can’t go to hospital for a skin condition in the middle of a pandemic, so I found a number and called my local hospital who told me to call 111, which I did, only to be told I needed to see my GP. It was just like going round in circles – back to square one. I’ve still not seen my GP.’
In the end, Mrs Payne was forced to pay for her own light-therapy treatment at a suntan booth.
She said: ‘Now my psoriasis has improved so much, I’m down to about 10 per cent – but not through any help from my GP.’
CASE STUDY THREE
Mouth cancer was missed because I couldn’t get a GP
Nicole Freeman is lucky to be alive after her mouth cancer was misdiagnosed because she couldn’t see her GP in person during the pandemic.
The 25-year-old was four months’ pregnant when she noticed a sore at the back of her tongue in November last year.
Unable to see her GP due to Covid restrictions, she had five phone conversations and sent photographs of the sore to her family doctor over five months. Each time she was told not to worry because it was an ulcer and she was prescribed Bonjela gel and medicated mouthwash.
It was only when hospital doctors looked at her tongue when she was in labour in March that they insisted on a biopsy and the cancer was diagnosed.
The mother of two, from York, said she was backing the Daily Mail’s campaign.
‘GPs need to start offering more face-to-face appointments,’ she said. ‘If I hadn’t been pregnant I would have been dead by now. My cancer would have been caught much quicker if I could have seen a doctor, instead of sending a picture. You just can’t tell from a picture what is going on.

Nicole Freeman is lucky to be alive after her mouth cancer was misdiagnosed because she couldn’t see her GP in person during the pandemic
‘To this day I still have to chase my GP for the simplest thing, such as my medications on repeat prescription. I’ve still had no face-to-face appointments with my GP even though we keep asking.’
Mrs Freeman – who has a second child called Holly, five – also suffers from a neurological condition. She said: ‘My health is rubbish at the moment and I’m in a lot of pain, which could be better managed if GPs were doing their jobs right. Instead we have to rely on the district nurse. I haven’t had any morphine to help with my pain for a week because they keep messing up.’
She also said she was ‘absolutely terrified’ when she was diagnosed with cancer, adding: ‘I just looked at my baby girl and cried – she was only a week old. It should have been a happy time but instead I was making every day with my baby count until I had to go into hospital for a month for surgery and treatment.’
Her husband Jake, 28, added: ‘It was really frustrating. We weren’t getting anywhere with the doctors – there was no support at all. The doctors said if Nicole hadn’t been pregnant and in the hospital to give birth she would’ve died by June.’
Three weeks after giving birth to Nevaeh, Mrs Freeman, who runs a charity for impoverished families with her husband, had a 15-hour operation to remove the tumour and she lost half of her tongue.
Surgeons used skin and veins from her left arm to rebuild her tongue. They also had to remove her lymph nodes in her neck after discovering the cancer had spread.
Mrs Freeman, who uses a wheelchair because of her neurological condition, spent four weeks recovering in intensive care, using a tracheotomy to breathe.
She had to learn how to talk and swallow again, before undergoing courses of chemotherapy and radiotherapy.
Phone patients 14% more likely to go to hospital in next 3 days
By Victoria Allen and Daniel Martin for The Daily Mail
Patients given remote GP appointments are more likely to end up going to hospital as emergency cases, a study has found.
Researchers looked at more than 116,000 people in England who had an appointment with a GP, then became so ill within the next three days that they had to be admitted to hospital.
Patients who spoke to a GP over the phone were 14 per cent more likely to take themselves to hospital and end up being admitted than those who had a face-to-face appointment.
The findings suggest doctors are more likely to miss signs of serious illness or patient deterioration when they do not see people.
The authors of the study by Imperial College London say the rise of new appointment types should be ‘carefully investigated’ because of the risk of unintended consequences.
The findings came as the Daily Mail yesterday set out its manifesto campaigning for more face-to-face consultations with GPs.

Patients who spoke to a GP over the phone were 14 per cent more likely to take themselves to hospital and end up being admitted than those who had a face-to-face appointment. The findings suggest doctors are more likely to miss signs of serious illness or patient deterioration when they do not see people
In the three days leading up to their emergency admission to hospital, patients are likely to show signs that their helath is deteriorating, the study said.
So researchers analysed 116,097 people, between April 2014 and the end of 2017 who had been in contact with their GP and went to hospital three days later.
They took themselves to hospital – rather than being sent by a doctor – suggesting symptoms had potentially been missed.
Even before Covid struck and remote consultations were rolled out widely, phone consultations made up almost one in five appointments for the people in the study. More than 23,000 out of 116,097 spoke to a GP on the phone.
People given only a telephone appointment were 14 per cent more likely to take themselves to hospital three days later than those seen in-person.
But those seen face-to-face then telephoned by a GP afterwards were 11 per cent less likely to do this, suggesting calls can play an important role in monitoring people after they have been seen.
Many GPs say telephone consultations are vital to manage demand, are preferred by some patients and work well to quickly deal with straightforward cases.
But the new findings ‘caution against reliance on telephone consultations in primary care’.
However, the authors say more research is needed to understand what may go wrong in some cases where people have spoken to their doctor over the phone.
The study, published in the British Journal of General Practice, found almost one in five GP patients who became emergency hospital patients had already been in hospital or had surgery in the previous 30 days.
Among more than 300million primary care consultations with non-hospital doctors in England each year, only around 2 per cent ever have an issue which could cause them harm, researchers stressed.
Some seen by a GP may also see their condition deteriorate rapidly afterwards which could not necessarily have been predicted.

Many GPs say telephone consultations are vital to manage demand, are preferred by some patients and work well to quickly deal with straightforward cases. But the new findings ‘caution against reliance on telephone consultations in primary care’
Professor Azeem Majeed, a practising GP and co-author of the study, said: ‘Telephone consultations play an important role in healthcare and, when combined with face-to-face appointments, can help patients manage their health well.
‘But it is essential the Government’s policy of expanding telephone consultations in March 2020 in response to the pandemic is carefully evaluated.’
He added: ‘It is also essential for the Government to urgently address workforce shortages and capacity issues in the NHS.’
Last night Dennis Reed of Silver Voices, a campaign group for the over-60s, said: ‘We’ve always said that remote consultations are inherently unsafe and this research provides solid backing for the Mail campaign.
‘It is common sense that remote consultations in some cases are going to miss key signs and key symptoms.’
Dr Richard Vautrey, chairman of the GP committee at the British Medical Association, said: ‘GPs are seeing millions of their patients face-to-face as well as offering telephone and online appointments every week.
‘The move to an initial telephone consultation was, and is, in line with NHS England’s and the Government’s guidance and is still necessary for infection control and to keep patients and healthcare staff as safe as possible.
‘No one wants to leave a surgery with an infection they did not attend with.’
Professor Martin Marshall, chairman of the Royal College of GPs, said: ‘We are still in a pandemic and there is still a need for some infection control measures.’
DR. RENEE HOENDERKAMP: Why do they think we’re called family doctors?
There were no obvious red flags when I spoke to a man with a long history of abdominal pain recently, but doctor’s instinct told me I needed to see him. I’m his GP, but he seemed embarrassed to be ‘bothering’ me.
He assumed it was his irritable bowel syndrome playing up – but this time the pain was really getting him down.
When I examined his abdomen, there was clearly more than IBS going on.
I called the surgeons at our local hospital and he was admitted. It turned out he had a ruptured appendix and underwent emergency surgery. He later wrote to me thanking me for saving his life.
That was one of the more dramatic cases of the day, but equally important was seeing an elderly lady who didn’t have anything much wrong with her, nor anything very new to say: she just needed a human being she trusted to sit and talk to.

In March 2020, GPs were told by the Government to ‘go digital’ and assess patients online, or in telephone consultations. Many are still rigidly following that guidance, even though the situation with Covid has changed. (Dr Renee Hoenderkamp, left, is an NHS GP)
That’s fine. It’s very much part of my job to reassure patients, especially ones who are frightened and have suffered terrible isolation over the past 18 months. So it is disturbing to think that some GPs have got used to keeping patients at a distance.
In March 2020, GPs were told by the Government to ‘go digital’ and assess patients online, or in telephone consultations. Many are still rigidly following that guidance, even though the situation with Covid has changed.
A lot of GPs seem to have embraced the change, as it allows them flexibility to work from home.
But many patients absolutely hate it. Fairly or otherwise, thousands have come to believe their GP has shut up shop.
Almost everyone seems to know someone who has spent hours trying to get through to their practice only to be told they have to communicate by email – or who has gone private out of desperation.
When Health Secretary Sajid Javid told MPs recently that it was ‘high time’ GPs got back to offering face-to face appointments, there was an indignant response from doctors who argued they were simply following official guidelines – and to be fair, they are.
That’s why it’s essential the Government changes those guidelines and issues a directive to GPs that face-to-face appointments should once again be the default (with the patient able to go virtual if they want to).
It’s also why I welcome the Daily Mail’s campaign supporting this urgently needed change.
Throughout the pandemic, the surgery where I work in north London has tried to continue as normally as possible, adapting as the Covid situation changed. We have maintained 15-minute fixed-time appointments, whether it’s by telephone or video. Too many surgeries vaguely offer to call people to discuss their symptoms later that day.
We started seeing patients in a more normal way about six months ago, though we do still have a system in place – and this isn’t my choice as I don’t run the practice – whereby a patient has to be triaged by a GP over the phone to determine whether they need to come in.
To me, that’s inefficient. If you do need to see the patient, they’ve got to book another appointment, so the first call on the phone is as good as wasted. I admit that when the Government advice to GPs to work remotely was first issued last March, it seemed sensible. We knew little about Covid then, and we did not have a vaccine.
I had a two-year-old daughter and my mother, 77, was looking after her during the day, so I was more than aware of the risk of picking up the virus and bringing it home.
GPs’ waiting rooms are always a breeding ground for disease, so the last thing we wanted was people sitting around giving each other Covid. But I was lucky – I’d trained at a surgery that did some emergency appointments over the telephone anyway, so I’d had plenty of experience of telephone triage. For a lot of GPs, phone consultation was a new skill entirely.
You don’t have any of the usual cues you get from a patient’s pallor or demeanour, so it’s all about rigorous questioning. I’ve picked up as many cancers over the telephone as I would normally. But I don’t think enough GPs have the same experience and, either way, it’s not always going to be a suitable approach. In many cases, vital symptoms will have been missed.
I realised just how bad the situation was at the peak of the pandemic, when I worked at Barnet Hospital as a front-of-house GP assessing patients as they arrived.

‘The irony is that most doctors become GPs because they like people. GPs aren’t known as ‘family doctors’ for nothing. We pride ourselves on knowing the people we care for. If we don’t get this crisis sorted, we risk losing touch with the very purpose of our work’
From listening to many of them, it was clear they were there because they felt it was impossible to see their GP. A 90-year-old woman told me she was only allowed to talk to hers now via ‘eConsult’, an online system she couldn’t understand.
All the patients I saw had fairly minor ailments such as knee pain, a minor allergy that had flared up that morning or a small complication with the contraceptive pill.
They were scared and unwell, but none of them needed to be at A&E. A quick conversation with their GP would have sorted the situation, but they all believed their GP was unavailable.
Clearly, we need to take action. But the pandemic isn’t totally behind us, so we have to think carefully about what we do next.
We know that while the vaccine is stopping people from dying, it’s not stopping people from catching and transmitting Covid. We’ve also all been cocooned for so long that as we go into winter all sorts of respiratory viruses will be waiting to take hold. Given all that, it still doesn’t make sense to fill up GP waiting rooms needlessly with vulnerable people.
So maybe the answer lies in patient choice. Let’s allow people to choose between a face-to-face appointment and a video or telephone consultation, having assessed their own risk and decided whether they want to come in.
I think patients would feel reassured if they knew they could see a doctor as a default. Otherwise it’s easy to feel palmed off.
The irony is that most doctors become GPs because they like people. GPs aren’t known as ‘family doctors’ for nothing. We pride ourselves on knowing the people we care for.
If we don’t get this crisis sorted, we risk losing touch with the very purpose of our work.
Dr Renee Hoenderkamp is an NHS GP
Source link : https://www.dailymail.co.uk/news/article-10010855/Boris-Johnson-urges-MPs-offer-person-consultations-patients.html