
5 Popular Foods That May Affect Your Health - Smarter Swaps for a Better Diet
5 Everyday Foods to Be Mindful Of - Healthier Choices Ahead
A mini-stroke, medically known as a transient ischemic attack (TIA), is often described as a “warning stroke.” Symptoms may last only a few minutes or hours and then completely disappear. Because there is no permanent damage in many cases, people frequently ignore it.
That is a dangerous mistake.
A TIA is not a harmless event. It is one of the strongest predictors of a future, potentially disabling stroke. For individuals in their 40s and beyond, a mini-stroke should be treated as a serious medical alarm — not an inconvenience that passed.
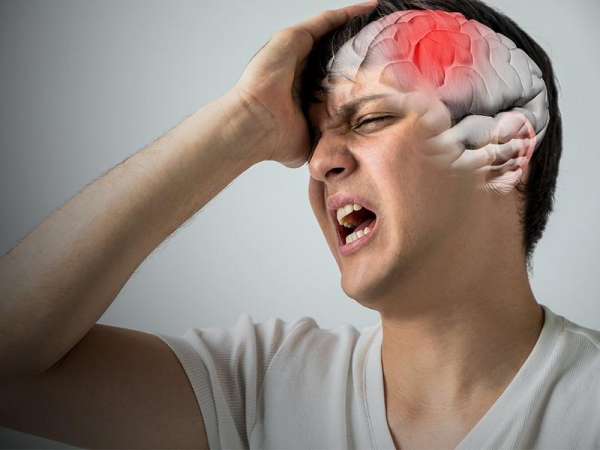
A transient ischemic attack occurs when blood flow to part of the brain is temporarily blocked. Unlike a full ischemic stroke, the blockage resolves before causing permanent tissue death.
However, the mechanism is the same:
A blood clot forms or travels to the brain.
Blood supply is reduced.
Brain cells are deprived of oxygen.
The difference is duration — not severity of risk.
Although strokes can happen at any age, risk rises significantly after 40 due to:
High blood pressure
Elevated cholesterol
Type 2 diabetes
Smoking
Sedentary lifestyle
Obesity
Chronic stress
Midlife is often when these risk factors quietly accumulate.
Many individuals feel generally healthy and overlook subtle symptoms, assuming they are “just tired” or “overworked.”
Symptoms often appear suddenly and may include:
Sudden numbness or weakness (especially on one side of the body)
Facial drooping
Difficulty speaking or slurred speech
Temporary vision loss in one eye
Blurred or double vision
Sudden dizziness or loss of balance
Confusion
The key characteristic is abrupt onset.
Even if symptoms resolve within minutes, the event still counts as a neurological emergency.

Research shows that:
Up to 1 in 3 people who experience a TIA will later have a full stroke.
The highest risk period is within the first 48 hours.
The first 90 days carry substantial danger.
A mini-stroke is not a “false alarm.” It is often the brain’s final warning before a major event.
There are several psychological reasons people dismiss TIAs:
Symptoms disappear quickly.
There is no pain.
There is no visible injury.
Individuals fear overreacting.
They attribute symptoms to fatigue or dehydration.
Unfortunately, waiting for symptoms to return can be life-altering.
A TIA signals that something in the vascular system is unstable.
Possible underlying causes include:
Narrowed carotid arteries
Atrial fibrillation (irregular heartbeat)
Blood clotting disorders
Uncontrolled hypertension
Plaque buildup in arteries
The event indicates that circulation to the brain has already been compromised.

When a TIA occurs in midlife (40s–60s), it often reflects years of silent vascular damage.
At this stage:
Arteries may be stiffening.
Plaque may be accumulating.
Metabolic dysfunction may be progressing.
A TIA at this age is frequently a signal that preventive measures were delayed — but it is still not too late to intervene.
If TIA symptoms appear:
Seek emergency medical care immediately.
Do not wait for symptoms to disappear.
Do not drive yourself if possible.
Doctors may perform:
Brain imaging (CT or MRI)
Carotid ultrasound
Heart rhythm monitoring
Blood clotting assessments
Early treatment may include:
Antiplatelet medications
Blood pressure control
Cholesterol-lowering therapy
Blood thinners for atrial fibrillation
Rapid intervention dramatically reduces future stroke risk.
A TIA provides a second chance.
Key prevention strategies include:
Hypertension is the leading stroke risk factor.
Reduce LDL cholesterol and increase HDL through diet and medication if necessary.
Diabetes significantly increases stroke risk.
Smoking accelerates vascular damage.
At least 150 minutes of moderate exercise per week.
Undiagnosed atrial fibrillation is a major cause of stroke.
Many individuals experience anxiety after a TIA. This emotional response is understandable.
However, fear can be reframed as motivation.
A mini-stroke is not just a medical event — it is an opportunity for intervention before permanent damage occurs.
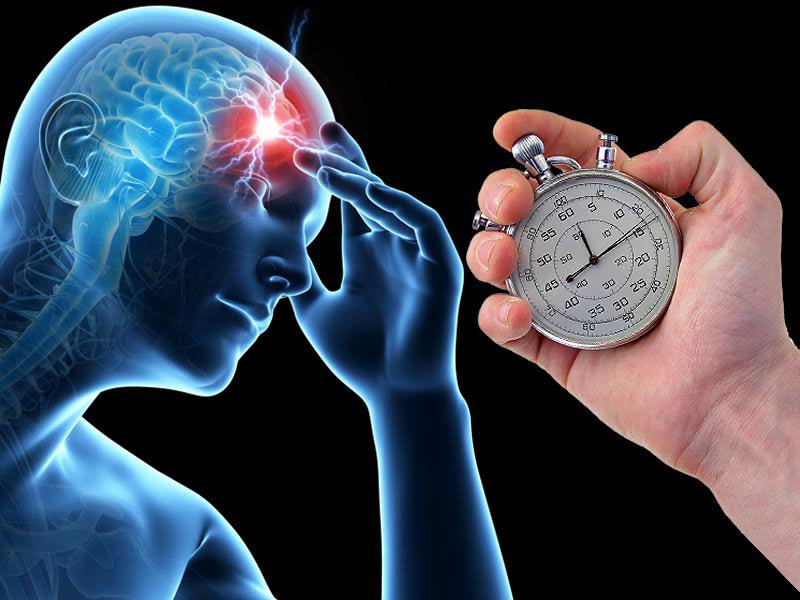
Medical professionals emphasize the FAST acronym:
Face drooping
Arm weakness
Speech difficulty
Time to call emergency services
Even if symptoms resolve, emergency evaluation remains critical.
A mini-stroke is silent because:
It may not leave visible damage.
It may not cause pain.
It may not disrupt daily function for long.
But beneath the surface, it reveals vascular instability.
Ignoring it increases the probability of a severe, potentially disabling stroke.
Mini-strokes in midlife and beyond are not minor events. They are urgent warnings.
They signal that blood flow to the brain has already been interrupted — even if temporarily.
For individuals in their 40s and older, a TIA should prompt immediate medical evaluation and serious lifestyle reassessment.
The brain often offers one warning before catastrophe.
Recognizing that red flag — and acting decisively — can mean the difference between prevention and permanent damage.
When it comes to stroke risk, time is not just important.
Time is brain.

5 Everyday Foods to Be Mindful Of - Healthier Choices Ahead
Feel Tired All the Time? It Might Be Your Circulation

How to Defrost Fish Safely: 3 Fast and Trusted Methods

She Ate Steamed Sweet Potatoes Every Day — But Her Liver Test Results Left Her in Sh.o.ck
Be Alert: Bruises in These Spots May Signal a Health Issue

Doctors Reveal Why Night Showers Beat Morning Showers Every Time

7 Surprising Signs You May Be Low on Vitamin B12 - Pay Attention

While Cucumbers Are Nutritious, Certain People Should Be Cautious

Why Chicken Feet Are a Healthy Choice You Shouldn’t Ignore?

Leftovers can be deadly—if they remain, throw them away immediately!
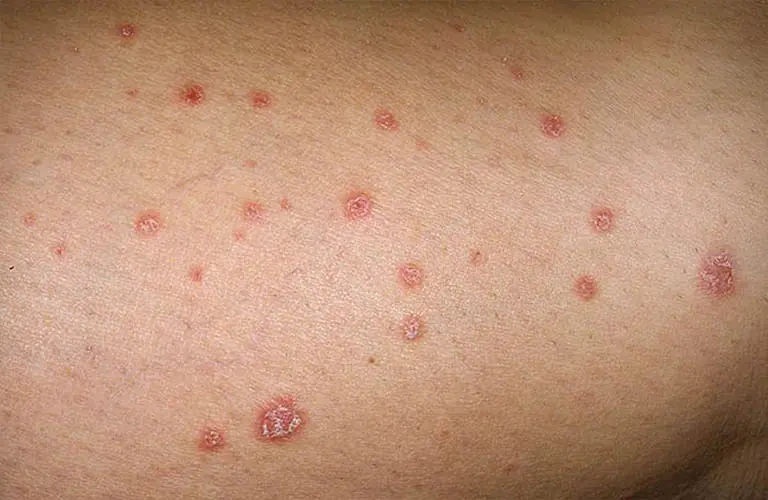
Tiny Red Dots on Your Skin: Possible Causes and Their Meanings
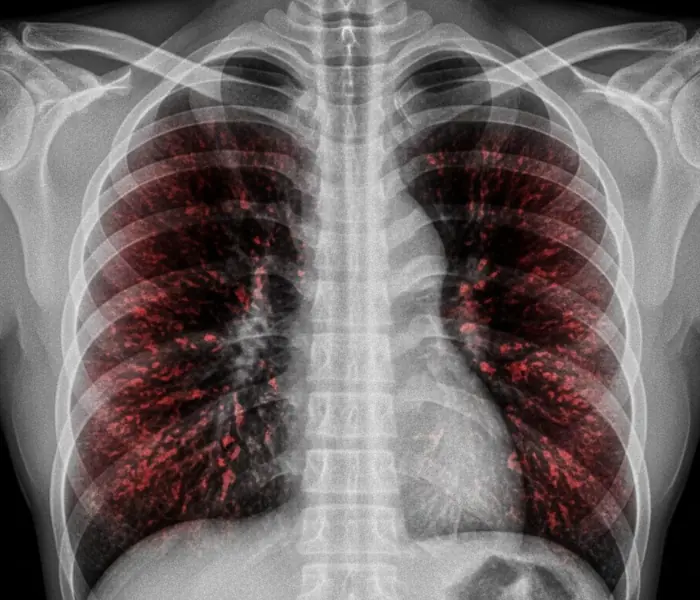
The Surprising Rise of Lung Can.cer in Non-Smokers and Its Possible Causes

5 Health Conditions That May Require You to Avoid Ginger

Banana Blossom Power: The Secret Superfood That Can Revitalize Your Body

When Punch Falls for Someone, He Acts Human… But That Might Be Only the Beginning

Too Much Burping? Your Body Might Be Warning You

If You’re Farting Excessively, Your Body Could Be Sending a Warning ⚠️ Find Out Why 👇
Sour Vaginal Smell? Here Are 4 Real Causes Every Woman Should Be Aware Of
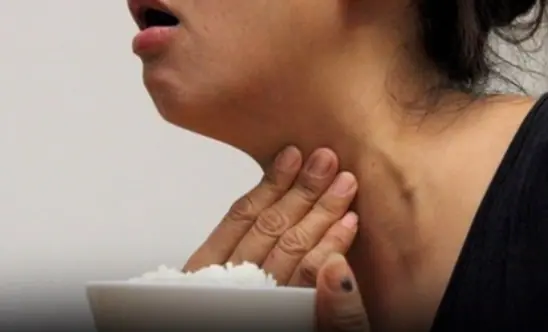
Conclusion Thyroid cancer may present with subtle or unexpected symptoms beyond the commonly known neck lump. Being aware of these signs — persistent hoarseness, difficulty swallowing, neck swelling, and more — can help you seek early diagnosis and

As one doctor noted: “Even healthy foods can have unintended effects if consumed without care. Moderation and attention to your body’s response are essential.”

5 Everyday Foods to Be Mindful Of - Healthier Choices Ahead

Feel Tired All the Time? It Might Be Your Circulation

How to Defrost Fish Safely: 3 Fast and Trusted Methods

She Ate Steamed Sweet Potatoes Every Day — But Her Liver Test Results Left Her in Sh.o.ck

Be Alert: Bruises in These Spots May Signal a Health Issue

Doctors Reveal Why Night Showers Beat Morning Showers Every Time
9 Everyday Items in Your Home That Could Affect Your Health

7 Surprising Signs You May Be Low on Vitamin B12 - Pay Attention

Keep your ginger fresh for months with simple methods that don’t require refrigeration or extra effort

While Cucumbers Are Nutritious, Certain People Should Be Cautious

Why Chicken Feet Are a Healthy Choice You Shouldn’t Ignore?

Leftovers can be deadly—if they remain, throw them away immediately!

Tiny Red Dots on Your Skin: Possible Causes and Their Meanings

The Surprising Rise of Lung Can.cer in Non-Smokers and Its Possible Causes

5 Health Conditions That May Require You to Avoid Ginger

Banana Blossom Power: The Secret Superfood That Can Revitalize Your Body

When Punch Falls for Someone, He Acts Human… But That Might Be Only the Beginning

Too Much Burping? Your Body Might Be Warning You

6 Surprising Reasons Luffa Is Better for You Than You Think

If You’re Farting Excessively, Your Body Could Be Sending a Warning ⚠️ Find Out Why 👇