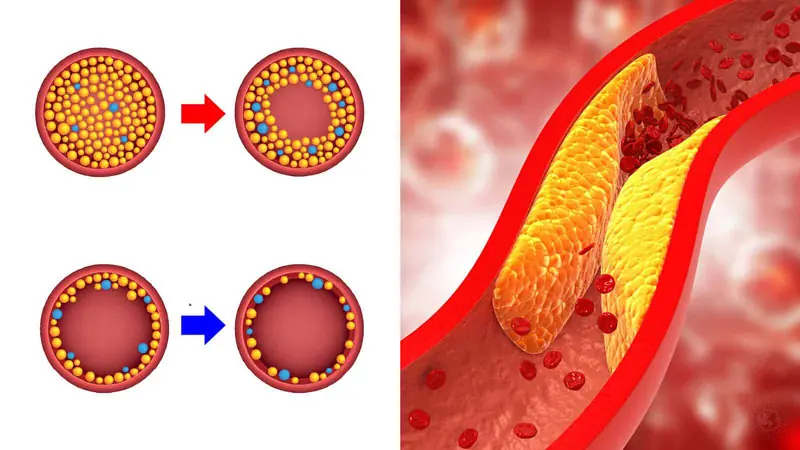
Diabetes is a chronic condition that affects how the body regulates blood sugar (glucose). When blood sugar levels remain elevated over time, they can damage blood vessels and nerves throughout the body. One of the areas most vulnerable to these changes is the feet.
Foot problems are common in people with diabetes, especially when blood sugar is not well controlled. Because circulation and nerve function are often affected, the feet can show early warning signs that should never be ignored.
Recognizing symptoms early and taking proper care can significantly reduce the risk of serious complications such as infections, ulcers, or even amputation. Below are 12 signs that diabetes may be affecting your feet.
1. Burning or Sharp Pain
A burning, stabbing, or shooting pain in the feet — particularly at night — may be a sign of diabetic neuropathy. This condition occurs when prolonged high blood sugar damages the nerves.
Damaged nerves can misfire, creating abnormal sensations such as:
-
Burning
-
Electric-like shocks
-
Sharp pain
-
Increased sensitivity to touch
These symptoms often begin gradually and may worsen over time if blood sugar levels remain uncontrolled.

2. Cold Sensation in the Feet
If your feet feel unusually cold even when the rest of your body feels warm, it could indicate poor circulation. Diabetes can narrow and damage blood vessels, reducing blood flow to the extremities.
Impaired circulation may cause:
-
Cold feet
-
Pale or bluish skin tone
-
Slower healing
Reduced blood flow limits oxygen delivery, which is essential for tissue health.
3. Numbness or Tingling
One of the most common early signs of diabetic neuropathy is numbness or a “pins and needles” sensation in the feet.
As nerves become damaged, they may lose the ability to transmit signals properly. This can result in:
-
Decreased sensation
-
Tingling
-
Loss of ability to feel pain or temperature
Loss of sensation is particularly concerning because injuries may go unnoticed.
4. Frequent Foot Cramps
Muscle cramps in the feet or lower legs may be linked to poor circulation or nerve damage. These cramps may occur during activity or at night and can be painful.
When muscles do not receive adequate oxygen-rich blood, cramping becomes more likely.

5. Slow-Healing Cuts or Sores
High blood sugar can interfere with the body’s natural healing processes. Even small cuts, blisters, or scratches on the feet may take longer than usual to heal.
Delayed healing increases the risk of:
-
Infections
-
Ulcers
-
Tissue damage
In severe cases, untreated wounds can become serious medical emergencies.
6. Changes in Skin Color
Poor circulation can lead to visible changes in the appearance of the skin on the feet. You may notice:
-
Redness
-
Bluish tint
-
Darkened areas
These changes may signal reduced blood supply and should be evaluated by a healthcare provider.
7. Dry, Cracked Skin
Diabetes can affect the skin’s ability to retain moisture. Dryness may lead to:
-
Peeling
-
Itching
-
Cracked heels
Deep cracks create openings where bacteria can enter, increasing infection risk.
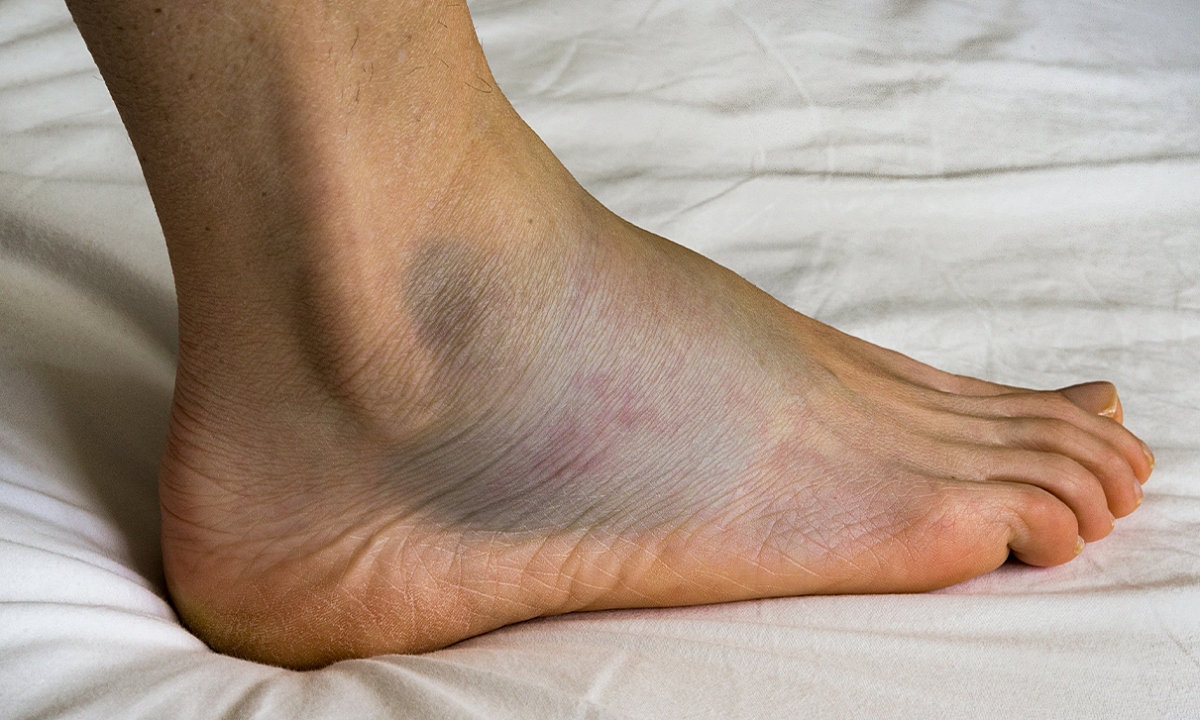
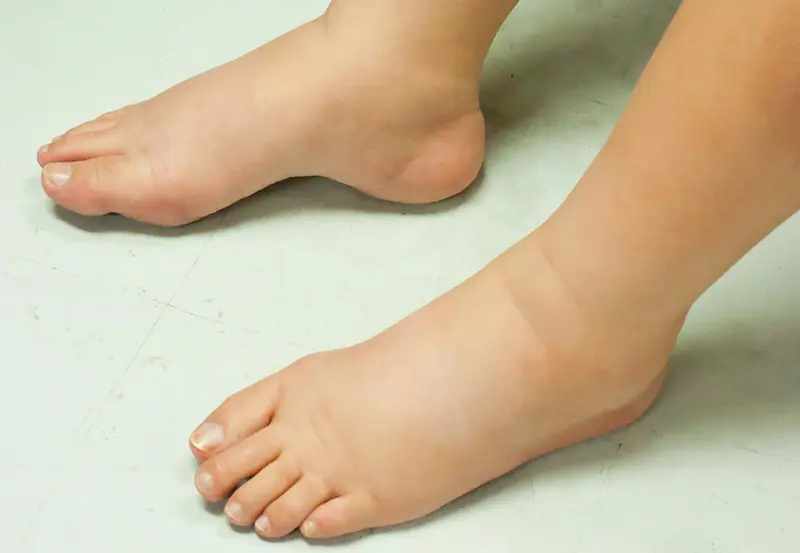
8. Swelling in the Feet or Ankles
Swelling may result from fluid retention or circulation issues. Persistent swelling can make walking uncomfortable and may indicate underlying vascular complications.
If swelling is sudden or severe, medical evaluation is necessary.
9. Fungal Infections
People with diabetes are more prone to fungal infections, especially in warm and moist areas like between the toes or under the toenails.
Common signs include:
-
Thickened or discolored toenails
-
Itching
-
Redness
-
Peeling skin
A weakened immune response makes infections harder to clear.
10. Foot Deformities
Long-term nerve damage can alter muscle balance in the feet, leading to structural changes such as:
-
Hammertoes
-
Claw toes
-
Bunions
These deformities may create pressure points that increase the risk of sores and calluses.
11. Blisters, Corns, and Calluses
Reduced sensation means blisters or calluses may develop without being noticed. Friction from poorly fitting shoes can cause skin breakdown.
Without proper care, these minor issues may progress into ulcers.
12. Changes in Toenail Appearance
Thickened, yellowed, brittle, or ingrown toenails are common among individuals with diabetes. Poor circulation and fungal infections often contribute to these changes.
Regular nail care is essential to prevent complications.
How to Protect Your Feet If You Have Diabetes
Proper foot care is a critical part of diabetes management. Simple daily habits can dramatically reduce complications.
1. Inspect Your Feet Every Day
Check for cuts, blisters, redness, swelling, or nail changes. Use a mirror to examine the soles if needed.
2. Keep Feet Clean and Dry
Wash daily with lukewarm water and mild soap. Dry thoroughly, especially between the toes.
3. Moisturize Carefully
Apply lotion to prevent dryness, but avoid the areas between the toes to prevent fungal growth.
4. Wear Well-Fitting Shoes
Choose shoes that fit properly and provide cushioning. Avoid tight footwear or walking barefoot.
5. Maintain Healthy Blood Sugar Levels
Consistent blood sugar control is the most effective way to prevent nerve damage and circulation problems.
6. Schedule Regular Foot Exams
Routine checkups with a healthcare provider or podiatrist can detect issues before they become severe.
Final Thoughts
Your feet can offer important clues about your overall health. In people with diabetes, changes in sensation, circulation, or skin condition may be early warning signs of complications.
Prompt attention to symptoms and consistent foot care can prevent serious outcomes. Diabetes management is not only about monitoring blood sugar — it also involves protecting vulnerable areas of the body, especially the feet.
If you notice any unusual changes, consult a healthcare professional promptly. Early intervention can make a significant difference in long-term health and quality of life.