
Itching in 9 Body Areas: When It May Signal a Serious Health Issue
When itching could signal more than dry skin
Stroke is often perceived as a sudden and unpredictable medical emergency. While strokes can occur without warning, research shows that long-term lifestyle patterns significantly influence risk. Many of these risk factors build gradually — and some of them are tied to nighttime routines.
Evening habits affect blood pressure regulation, heart rhythm stability, blood sugar control, and sleep quality. Because the body undergoes important cardiovascular and neurological adjustments during sleep, unhealthy nighttime behaviors can quietly increase strain on the brain and blood vessels.
Below are five nighttime habits that medical professionals frequently caution against, along with explanations of why they matter.
Sleep is not simply rest — it is a biological reset period. During deep sleep, blood pressure naturally declines, heart rate stabilizes, and the brain clears metabolic waste.
When individuals consistently sleep too little or stay up late:
Blood pressure may remain elevated overnight
Stress hormones such as cortisol increase
Inflammation markers rise
Blood vessel repair is impaired
Chronic sleep deprivation has been linked to hypertension, diabetes, obesity, and atrial fibrillation — all major stroke risk factors.
Most adults require 7–9 hours of quality sleep. Regularly sleeping less than six hours may significantly increase cardiovascular strain.

Eating large or high-sodium meals close to bedtime places extra stress on the cardiovascular and digestive systems.
Potential effects include:
Elevated nighttime blood pressure
Poor glucose control
Increased triglyceride levels
Disrupted sleep quality
Late-night meals high in salt can worsen fluid retention, contributing to hypertension. High sugar intake before sleep may impair insulin sensitivity and metabolic stability.
Ideally, the final meal should occur at least two to three hours before bed and be moderate in portion size.
Alcohol is commonly used as a relaxation aid, but it can significantly affect stroke risk.
Evening drinking may:
Raise blood pressure
Trigger irregular heart rhythms (such as atrial fibrillation)
Increase clotting tendency
Disrupt deep sleep stages
While moderate alcohol intake may be acceptable for some individuals, heavy or binge drinking — particularly at night — is strongly associated with both ischemic and hemorrhagic stroke.
Alcohol also interferes with restorative sleep cycles, compounding cardiovascular strain.
Sleep apnea is a condition in which breathing repeatedly stops and starts during sleep. It is a significant and often undiagnosed stroke risk factor.
When lying flat on the back:
Airway collapse becomes more likely
Oxygen levels fluctuate
Blood pressure surges occur repeatedly
The heart experiences rhythm disturbances
Over time, untreated sleep apnea increases the risk of hypertension, atrial fibrillation, and stroke.
Symptoms of sleep apnea include loud snoring, gasping during sleep, and excessive daytime fatigue. Medical evaluation and appropriate treatment (such as CPAP therapy) can significantly reduce risk.

Evening stress and excessive screen use can disrupt circadian rhythms and sympathetic nervous system regulation.
Exposure to blue light from phones or tablets suppresses melatonin production, delaying sleep onset. Psychological stimulation from social media or work-related tasks can keep stress hormones elevated.
Consequences may include:
Reduced sleep duration
Poor sleep quality
Elevated nighttime blood pressure
Increased systemic inflammation
Chronic stress is closely linked to cardiovascular disease. When stress remains active at bedtime, the body does not fully shift into its restorative state.
Blood pressure naturally follows a pattern known as “nocturnal dipping,” where it decreases during sleep. Individuals who do not experience this drop — often due to poor sleep habits — may have higher long-term stroke risk.
Sleep is also when:
The brain clears metabolic waste
The heart rate stabilizes
Hormonal balance is restored
Vascular repair occurs
Disrupting these processes night after night may gradually elevate cardiovascular strain.

Doctors often recommend simple adjustments to protect cardiovascular health:
Maintain a consistent sleep schedule
Aim for 7–9 hours of quality sleep
Avoid heavy meals within 2–3 hours of bedtime
Limit alcohol intake
Reduce evening screen exposure
Seek evaluation for snoring or suspected sleep apnea
Practice calming routines before sleep
Small improvements in nighttime routines can have cumulative long-term benefits.
Stroke risk does not develop overnight, but nightly habits contribute to long-term vascular health. Many behaviors that feel harmless — staying up late, scrolling in bed, late snacking, or heavy drinking — can influence blood pressure, heart rhythm, and inflammatory processes.
The goal is not fear, but awareness. Nighttime is when the body repairs and recalibrates. Supporting that process through consistent, healthy routines may reduce cardiovascular strain and protect brain health over time.
Sometimes, prevention begins not during the day — but in the hours before sleep.

When itching could signal more than dry skin
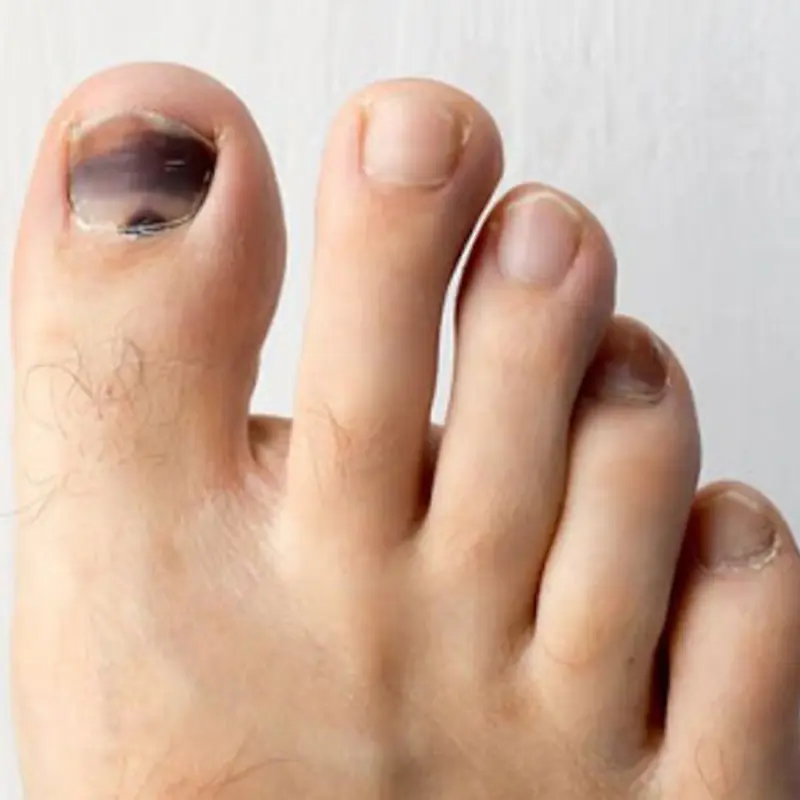
Why your toenail turns black — and what to do next

Bulging Veins: What Your Body Is Trying to Tell You — and When to See a Doctor
Back pain, urinary incontinence, then I'm sorry you have this terrible disease.
The earlier you catch it, the greater your chances of beating it — quickly and confidently

Eat these 8 foods to cut your risk of heart disease and cancer—doctor-approved
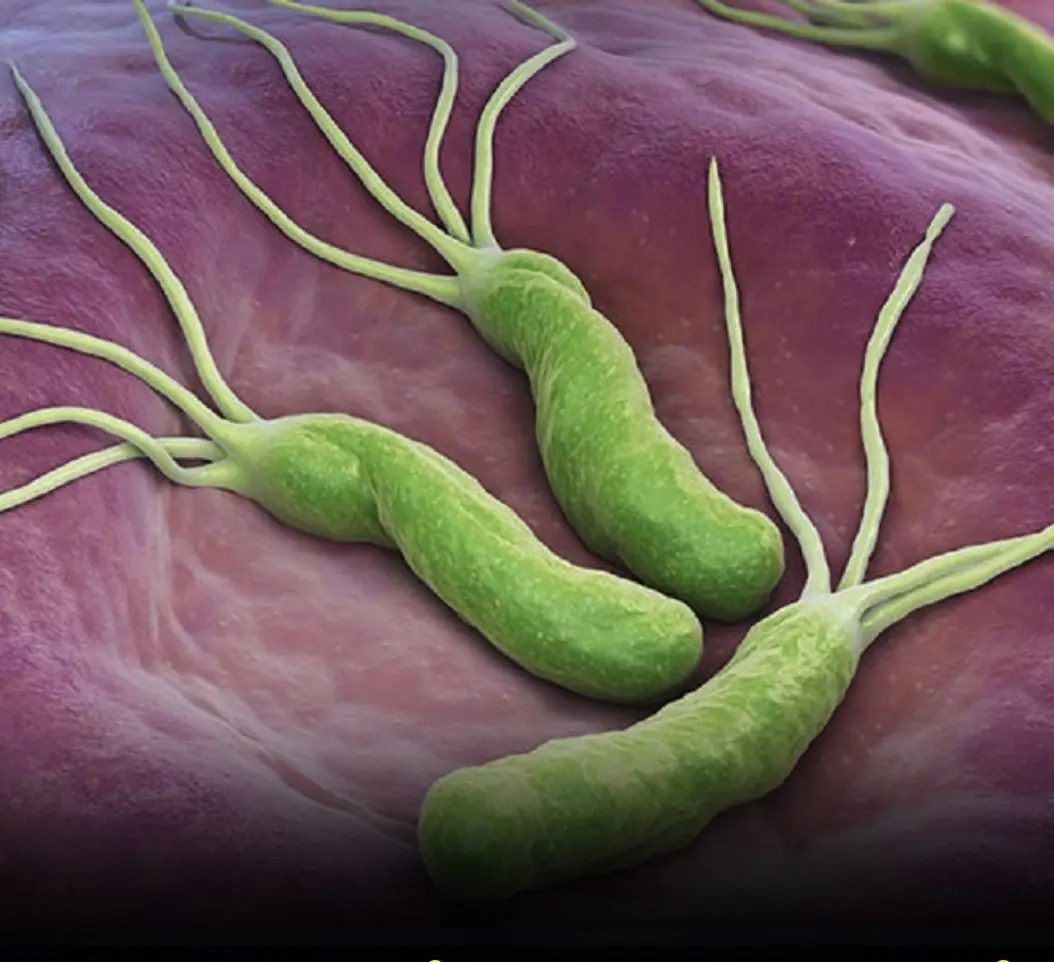
How to Treat H. Pylori (Helicobacter Pylori) Naturally Without Antibiotics.....

Only 1 spoon a day — this ‘blood-boosting superfood’ can make your skin glow

Not all fish are healthy: These 3 types may quietly raise cancer risk

What happens when you eat boiled eggs every morning?

The Advantages of Sleeping on Your Left Side

5 unusual symptoms that could signal hidden diabetes.
Add these 8 foods to help lower cancer risk naturally.

Not just forgetfulness — 6 early signs of dementia families often miss.

Ginger is healthy—but not ideal for certain conditions.
6 warning symptoms of early-stage colon can.cer you need to take seriously

Can You Eat Too Many Tomatoes? What You Should Know

It’s fragrant, refreshing, and a staple in many Southeast Asian kitchens
5 everyday foods that could potentially harm women’s ut.erine health

When itching could signal more than dry skin

My “Golden Child” Sister Tried to Turn My First Home Into Her Family’s Free Ride

The hidden home appliance driving up your power bill

A “Family Weekend” That Turned Into a Lesson They Won’t Forget

A Signature, a Family Secret, and the $9.8 Million Silence

Why your toenail turns black — and what to do next

Bulging Veins: What Your Body Is Trying to Tell You — and When to See a Doctor

Back pain, urinary incontinence, then I'm sorry you have this terrible disease.

The earlier you catch it, the greater your chances of beating it — quickly and confidently

Eat these 8 foods to cut your risk of heart disease and cancer—doctor-approved

How to Treat H. Pylori (Helicobacter Pylori) Naturally Without Antibiotics.....

Only 1 spoon a day — this ‘blood-boosting superfood’ can make your skin glow

Not all fish are healthy: These 3 types may quietly raise cancer risk

Garlic ranks only 9th… the No.1 longevity food is cheap, familiar, and already in your kitchen

Combining Lemon and Cloves: A Natural Pairing With Practical Daily Uses

What happens when you eat boiled eggs every morning?

The Advantages of Sleeping on Your Left Side

5 unusual symptoms that could signal hidden diabetes.

Add these 8 foods to help lower cancer risk naturally.