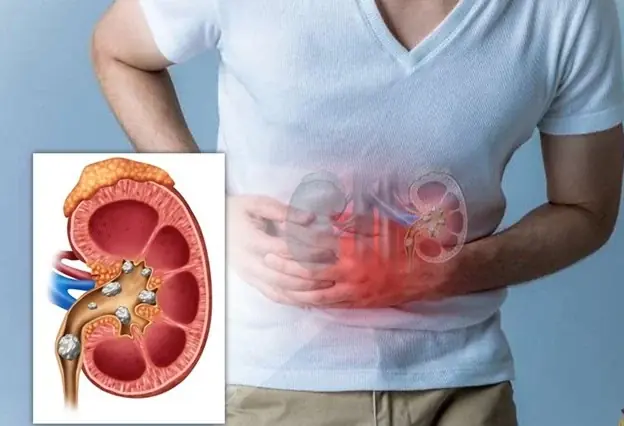
Signs your kidneys may not be functioning well – what to watch for
How to recognize early signs of kidney issues in your body
For most people in the United States, tuberculosis (TB) might seem like a disease of the past—something out of history books or 19th-century sanatoriums. But in Kansas, public health officials are confronting a stark reminder that TB is still very much a threat. A recent outbreak in the state has become the largest recorded in U.S. history, with dozens of confirmed and suspected cases, sending ripples of concern through the medical community.
Unlike the common cold or flu, TB doesn’t spread quickly or loudly. It lingers, sometimes silently, within infected individuals before making itself known—often after months or even years. This slow-moving but deadly nature makes outbreaks particularly alarming, as they often go undetected until they’ve spread far beyond their point of origin.
Kansas has now found itself at the center of the largest tuberculosis (TB) outbreak ever recorded in U.S. history. According to health officials, dozens of confirmed and suspected cases have surfaced, marking an alarming increase in a disease that has long been considered under control in the country. While public health authorities continue their investigations, the sheer scale of this outbreak has sparked widespread concern, not only for those directly affected but also for the potential of broader transmission. Unlike highly contagious respiratory illnesses like the flu or COVID-19, TB spreads more slowly, often simmering undetected within communities before reaching a tipping point—making outbreaks like this particularly challenging to trace and contain.
While the exact demographics of those infected have not been fully disclosed, certain risk factors make some populations more vulnerable to tuberculosis. Individuals with weakened immune systems, such as those with HIV/AIDS or diabetes, are at higher risk of developing active TB. Additionally, those living in close quarters, including nursing home residents, prison populations, and people experiencing homelessness, are more susceptible to rapid transmission. If the outbreak is affecting one of these high-risk groups, containment efforts could prove particularly difficult.
This situation stands in stark contrast to the overall trajectory of tuberculosis in the U.S. In recent decades, TB cases have steadily declined due to advances in medical treatment, improved public health surveillance, and rigorous screening programs. The Centers for Disease Control and Prevention (CDC) reported that in 2020, cases fell to a historic low, with fewer than 10,000 reported nationwide. However, experts caution that these statistics may have created a false sense of security. While TB is preventable and treatable, gaps in early detection, limited access to healthcare, and reduced routine screenings during the COVID-19 pandemic may have contributed to this resurgence.
The Kansas outbreak serves as a stark reminder that tuberculosis remains a public health threat—one that demands vigilance, swift intervention, and a better understanding of how and why this outbreak escalated to record-breaking proportions. As officials work to trace its origins, a critical question looms: How did this outbreak go undetected for so long?
Although tuberculosis (TB) may seem like a relic of the past, it remains one of the world’s deadliest infectious diseases, claiming over a million lives globally each year. Unlike the flu or COVID-19, which spread rapidly through casual contact, TB is a slow-moving but persistent bacterial infection that primarily affects the lungs. It is caused by Mycobacterium tuberculosis, a bacterium that spreads through airborne droplets when an infected person coughs, sneezes, speaks, or even sings. However, TB is not as easily transmissible as many other respiratory infections—prolonged exposure in enclosed spaces is typically required for the bacteria to take hold in another person.
There are two forms of tuberculosis: latent TB infection (LTBI) and active TB disease. The vast majority of people who contract M. tuberculosis never develop symptoms because their immune system successfully suppresses the bacteria, leaving them with latent TB. In this dormant state, the bacteria remain in the body without causing illness and are not contagious. However, about 5-10% of infected individuals will eventually develop active TB disease, particularly if their immune system is weakened due to factors such as malnutrition, chronic illness, or advanced age. Once TB becomes active, it can cause a range of debilitating symptoms, including persistent coughing, fever, night sweats, chest pain, fatigue, and weight loss. If left untreated, TB can be fatal.
One of the key challenges in controlling tuberculosis is that infected individuals may unknowingly carry the bacteria for months or even years before it progresses to an active, contagious state. This means that outbreaks, like the one in Kansas, often remain hidden until a cluster of cases emerges. TB outbreaks tend to occur in communities where people live in close proximity, such as nursing homes, correctional facilities, shelters, or densely populated households. Factors such as delayed diagnosis, lack of routine screening, and reduced public health resources can allow TB to spread undetected until the infection has already established a foothold.
The Kansas tuberculosis outbreak didn’t make headlines overnight. Like many TB outbreaks, it likely began with isolated cases that went undetected or were misdiagnosed as less serious respiratory illnesses. Unlike fast-spreading diseases such as influenza or COVID-19, tuberculosis moves slowly, often lingering in a community before an outbreak is officially recognized. By the time health officials confirmed the scope of the Kansas outbreak, dozens of cases had already surfaced, making it the largest recorded TB outbreak in U.S. history.
Early detection of tuberculosis is challenging because its symptoms can be mild at first and resemble common illnesses like bronchitis or pneumonia. A persistent cough, fatigue, and night sweats might not immediately raise alarm, particularly if a person doesn’t have known risk factors for TB. This can lead to delays in diagnosis, allowing the bacteria to spread unnoticed. In many cases, TB isn’t identified until multiple people in a community start showing symptoms, prompting further investigation.
Health officials in Kansas have not disclosed the exact moment the outbreak was first flagged, but once TB is suspected in multiple individuals, public health agencies typically act quickly. This involves extensive testing of close contacts, including family members, coworkers, and others who may have been exposed. Since TB can remain latent for months or even years, identifying all potential cases requires tracing back possible points of exposure over a long period.
The outbreak’s size suggests that TB may have been circulating within a specific community or institution before being detected. Schools, long-term care facilities, and correctional institutions are common settings for TB outbreaks because of prolonged close contact among individuals. While officials continue their investigation, one critical question remains: Why was this outbreak able to reach such unprecedented levels before it was fully recognized? The answer may lie in gaps within routine TB screening, shifts in public health priorities, or delays in treatment access.
Once tuberculosis was confirmed as the cause of the outbreak in Kansas, public health officials moved swiftly to contain its spread. Unlike viral outbreaks, which often rely on mass vaccination campaigns or broad public health restrictions, controlling TB requires a more targeted, multi-step approach. The primary focus is identifying infected individuals, treating active cases, and preventing latent infections from progressing into contagious disease. Given the scale of the outbreak, this effort has required significant coordination between local health departments, the Centers for Disease Control and Prevention (CDC), and healthcare providers.
A key part of the response has been extensive contact tracing, where health officials track down individuals who may have been exposed to a TB-positive person. This process involves testing family members, coworkers, and anyone who had prolonged close contact with confirmed cases. Because TB can remain dormant for months or years, officials are likely working to determine how far back exposure may have occurred and whether cases are linked to a common source, such as a specific facility or workplace.
Once infected individuals are identified, they are categorized into two groups: those with active TB disease, who require immediate treatment and isolation, and those with latent TB infection, who may not yet be sick but still need preventive therapy. Active TB cases are typically treated with a six-month regimen of antibiotics, often including drugs like isoniazid and rifampin. For latent infections, a shorter course of preventive antibiotics can significantly reduce the risk of the disease becoming active. However, TB treatment requires strict adherence, as failing to complete the full antibiotic course can lead to drug-resistant strains, making future treatment far more complicated.
The Kansas tuberculosis outbreak has highlighted significant vulnerabilities in the U.S. public health system, raising urgent questions about TB prevention, detection, and treatment. While TB cases in the country have been on a long-term decline, this record-breaking outbreak serves as a stark reminder that the disease has not been eradicated—and that under the right conditions, it can spread silently before reaching crisis levels.
One of the biggest concerns stemming from this outbreak is whether routine TB screening and surveillance efforts have weakened over time. Historically, TB control programs in the U.S. have been highly effective, relying on active case monitoring, targeted testing, and robust treatment protocols. However, the COVID-19 pandemic strained public health resources, diverting attention away from TB detection and prevention. Many routine screenings, particularly in high-risk populations, were delayed or deprioritized, potentially allowing latent TB infections to go unnoticed and progress into active cases. This shift in priorities may have contributed to the delayed recognition of the Kansas outbreak.
Additionally, access to healthcare remains a major barrier to TB control. The disease disproportionately affects marginalized communities, including individuals experiencing homelessness, those in correctional facilities, and people with limited access to medical care. These populations often face delays in diagnosis and treatment, increasing the risk of unchecked transmission. The Kansas outbreak underscores the need for improved healthcare access, routine screenings, and stronger outreach programs in vulnerable communities.
Another growing concern is the threat of drug-resistant tuberculosis. While no reports indicate that drug-resistant strains are involved in this outbreak, improper or incomplete treatment of TB can lead to antibiotic resistance, making future cases much harder—and more expensive—to treat. The outbreak serves as a crucial reminder of the importance of strict adherence to treatment regimens and the potential consequences of medication shortages or treatment interruptions.

How to recognize early signs of kidney issues in your body

How often should you take a shower?

Are Walnuts Good for You? Doctors Reveal the Answer…

Don’t Ignore THESE Symptoms—Your Kidneys Could Be at Risk

Thoughtful words matter most when comforting grieving families.
Subtle body signals may reveal hidden heart problems early.

Papaya seeds may offer surprising health benefits you never knew.
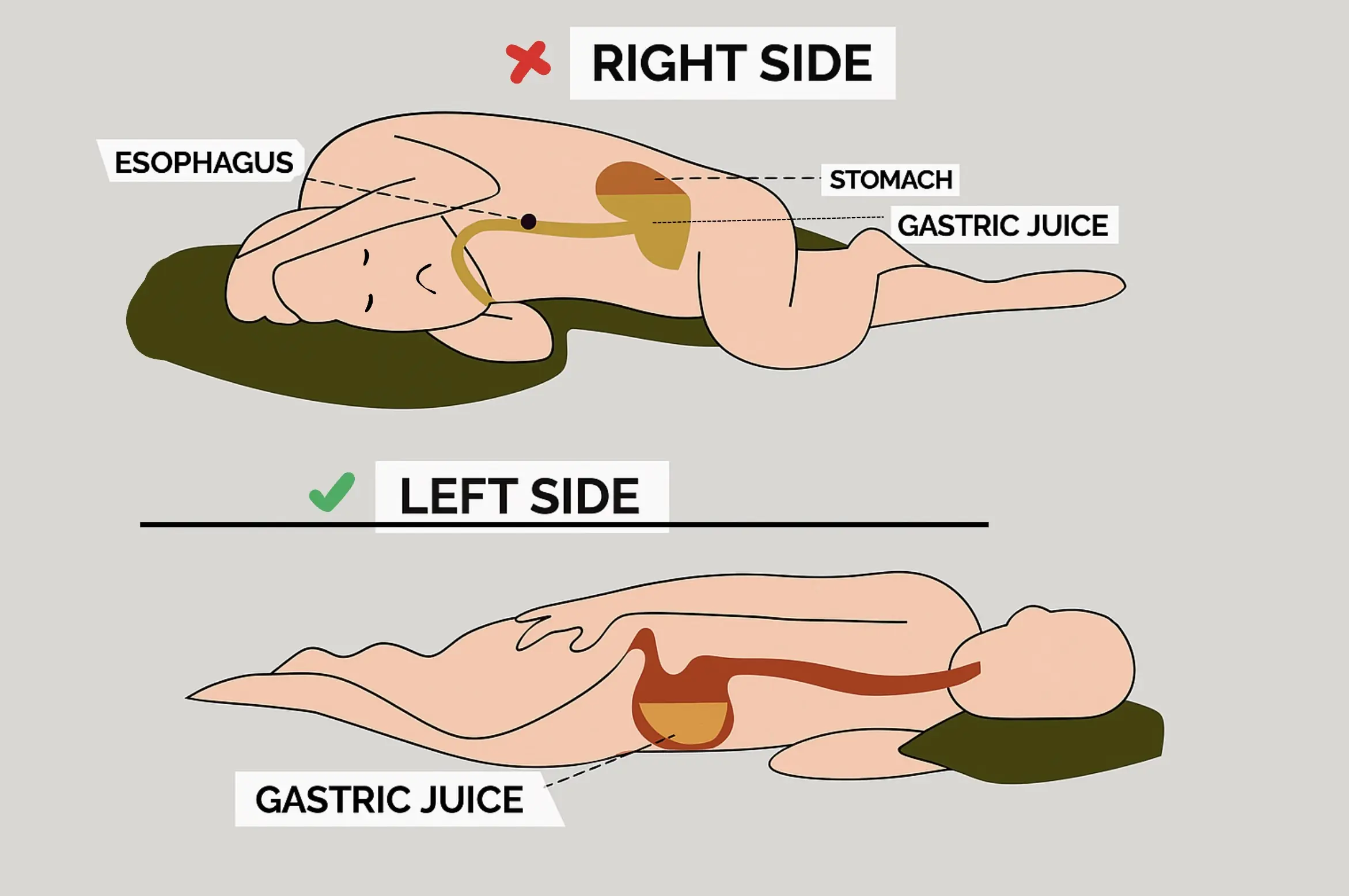
What Happens When You Sleep on Your Left Side Every Night?
Your Nighttime Routine Might Be Putting Your Health at Risk

What Happens When You Drink Water First Thing Every Day?

Who Should Avoid Ginger? 5 Health Conditions to Watch Carefully
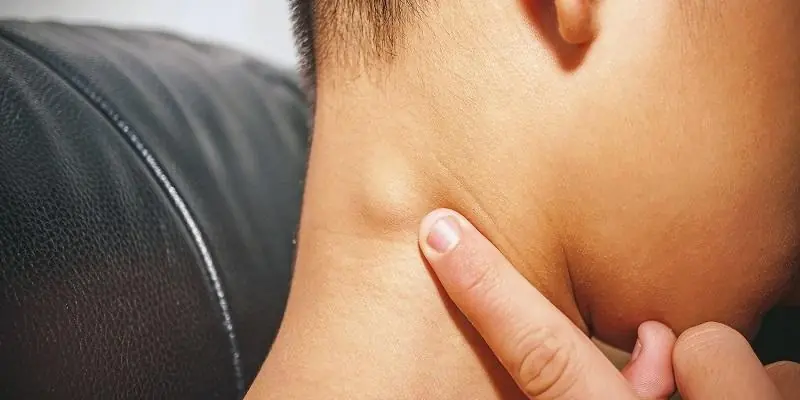
A neck lump can signal infection or more serious conditions—know signs.
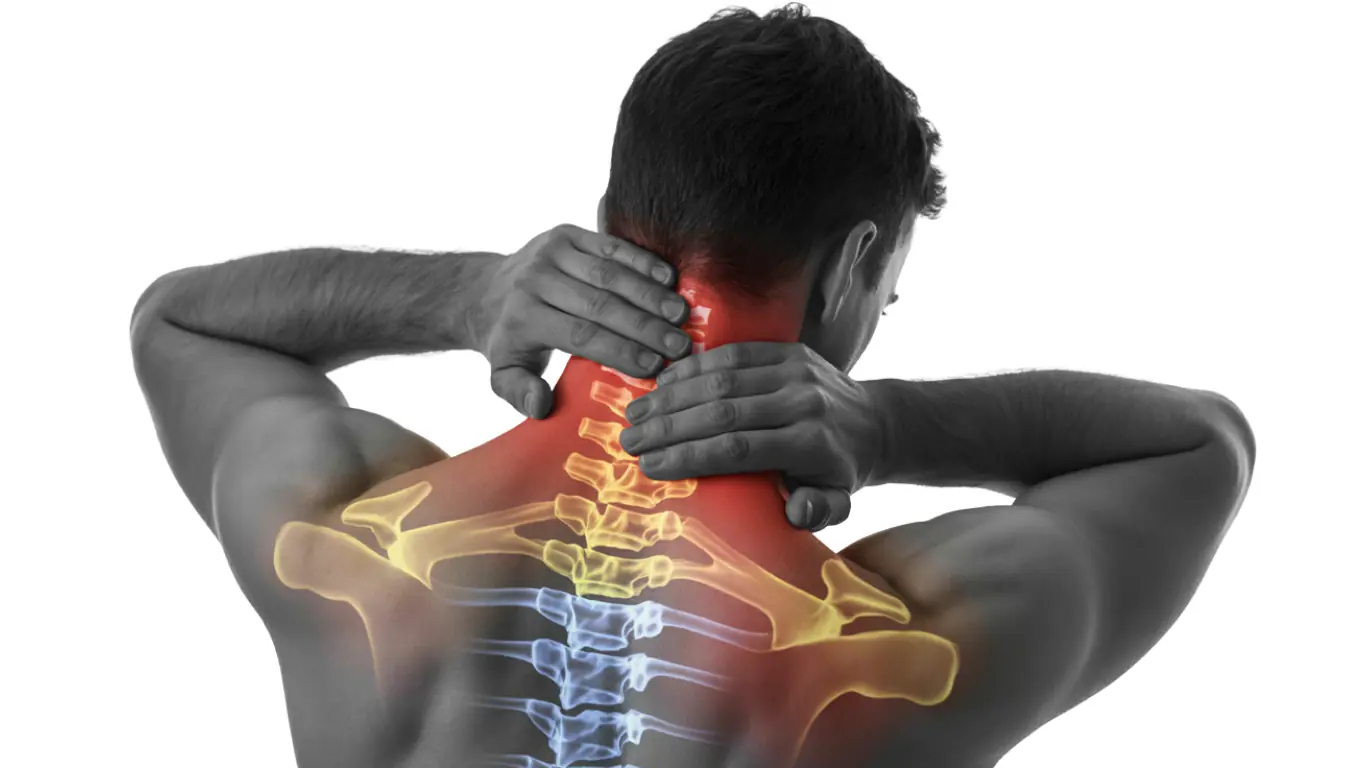
Stop Doing These 6 Things If You Have Neck Pain—They Could Be Harmful

20 impressive health benefits of sweet potatoes you should know

Amazing tomato facts that might shock you

Waking up several times at night to urinate? It may be more than just a routine habit

It’s Not the Eggs: The Hidden Habit That Could Turn Deadly

Doctors report a 36-year-old woman di.ed from diabetes despite not eating sugar

Doctors warn that everyday eating habits may contribute to serious diabetes complications

Morning boiled eggs may affect health—facts you should know today.

How to recognize early signs of kidney issues in your body

How often should you take a shower?

Are Walnuts Good for You? Doctors Reveal the Answer…

Don’t Ignore THESE Symptoms—Your Kidneys Could Be at Risk

Thoughtful words matter most when comforting grieving families.

Subtle body signals may reveal hidden heart problems early.

Papaya seeds may offer surprising health benefits you never knew.

What Happens When You Sleep on Your Left Side Every Night?

Your Nighttime Routine Might Be Putting Your Health at Risk

What Happens When You Drink Water First Thing Every Day?

Who Should Avoid Ginger? 5 Health Conditions to Watch Carefully

A neck lump can signal infection or more serious conditions—know signs.

Stop Doing These 6 Things If You Have Neck Pain—They Could Be Harmful

20 impressive health benefits of sweet potatoes you should know

Try placing ginger next to your pillow before bed – a small tip that could benefit your sleep

Amazing tomato facts that might shock you

Waking up several times at night to urinate? It may be more than just a routine habit

It looks like magic…

It’s Not the Eggs: The Hidden Habit That Could Turn Deadly

Doctors report a 36-year-old woman di.ed from diabetes despite not eating sugar